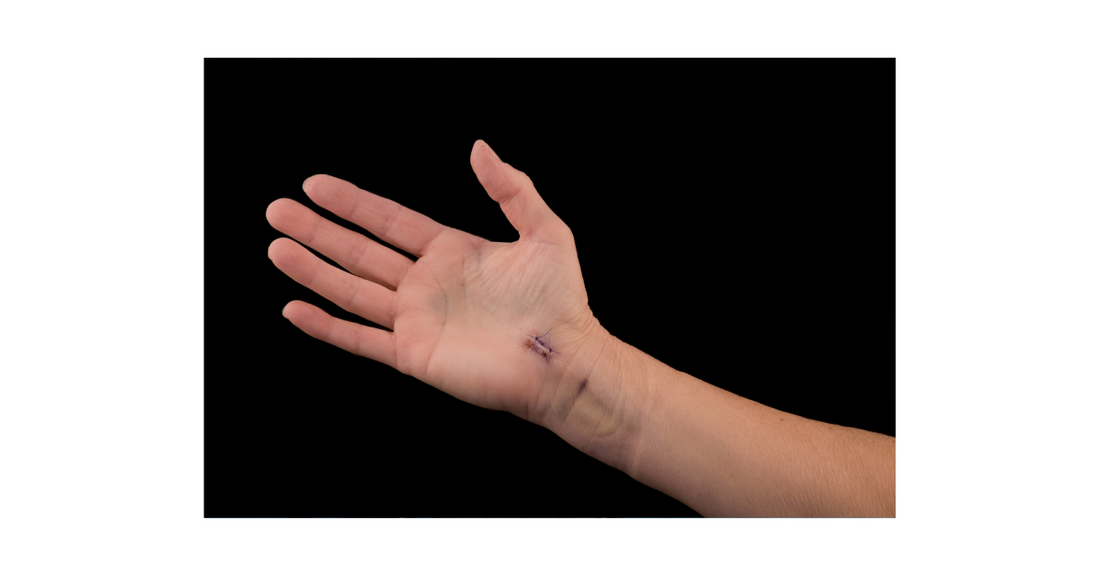
When, where, and who should treat Dupuytren's Contracture?
Getting a diagnosis of Dupuytren's contracture may be as simple as having a doctor look at your hand. However, there are also imaging techniques such as magnetic resonance imaging (MRI) and ultrasound as well as tissue examinations that can be done to confirm the condition.
If you have already been diagnosed with Dupuytren's, you may wonder what's next and who will treat your condition. While some treatments are evidence-based, there is still a lot of work to be done in the research arena. Doctors should use their clinical judgment to make the recommendation that's best for you. We'll discuss some common lines of treatment below.
Who should provide Dupuytren's treatment and where is it done?
The question of who is authorized to treat Dupuytren's contracture varies according to your country. In many cases, licensed rheumatologists (doctors who specialize in arthritis along with other joint and tissue conditions) are the best provider to seek care from. But some general providers may be brave enough to perform a percutaneous needle aponeurotomy, which may be indicated for you. Still, general practitioners and rheumatologists are equally unprepared to deal with complications of this condition.
Some countries require providers to have diplomas in hand surgery to perform operations for Dupuytren's. In other places, this condition can be treated by general surgeons, orthopedic surgeons, and plastic surgeons. But, generally, surgeons are good to consult with, especially if your case is severe.
Depending on financing, national regulations, your personal medical history, and other variables, the procedure can be done as an outpatient surgery (where you go home the same day) or you may spend up to one week in the hospital.
Surgical and non-surgical treatment options
Treatment for Dupuytren's contracture should start shortly after symptoms arise. If you wait for the nodular stage of the disease, surgery may not have great outcomes. Getting treatment is better than not getting treatment, but it's ideal to do it as early as possible.
There are non-surgical treatment options, including a collagenase injection and soothing creams to manage symptoms. In other countries, light therapy, acupuncture, ultrasound, and massage are recommended for the same purpose. Radiotherapy can sometimes be beneficial, especially at the start of the condition.
There are different types of surgery. Some doctors prefer to cut the affected cord and leave the remainder as is. Other surgeons may remove the cord after cutting or remove the cord along with surrounding healthy tissue. There are also various surgical styles that improve cosmetic appearance of the hand.
What happens after surgery?
After surgery, doctors give you one of the following post-operative approaches:
- Rehabilitation therapy from an occupational therapist/OT, physical therapist/PT, or certified hand therapist (who may also be a PT or OT); this includes early use of the affected hand via graded and progressive strengthening exercises, massage, edema management (reduction of swelling), and participation in self-care tasks where the hand is used safely and efficiently
- Using a standard protective splint (also known as an orthosis) during the day and night for the first one to two weeks; if healing is going well and there are no complications noted, doctors will recommend the splint be worn only at night for several more weeks or months to protect the hand and the surgical incision
- Dynamic splinting, which involves a device with a rigid bottom part to support the hand along with a movable aspect such as an elastic or pulley; this type of splinting is recommended for people who previously experienced severe immobility of the hand, as dynamic splints offer protection along with gradual and gentle increases in range of motion with the help of movable components
According to what we know about recovery after surgery, all three approaches are equally useful and effective parts of the rehabilitation process. However, doctors decide which to use according to the patient's condition, needs, and their medical history.
Learn More